10 early signs it’s time for professional dementia care 
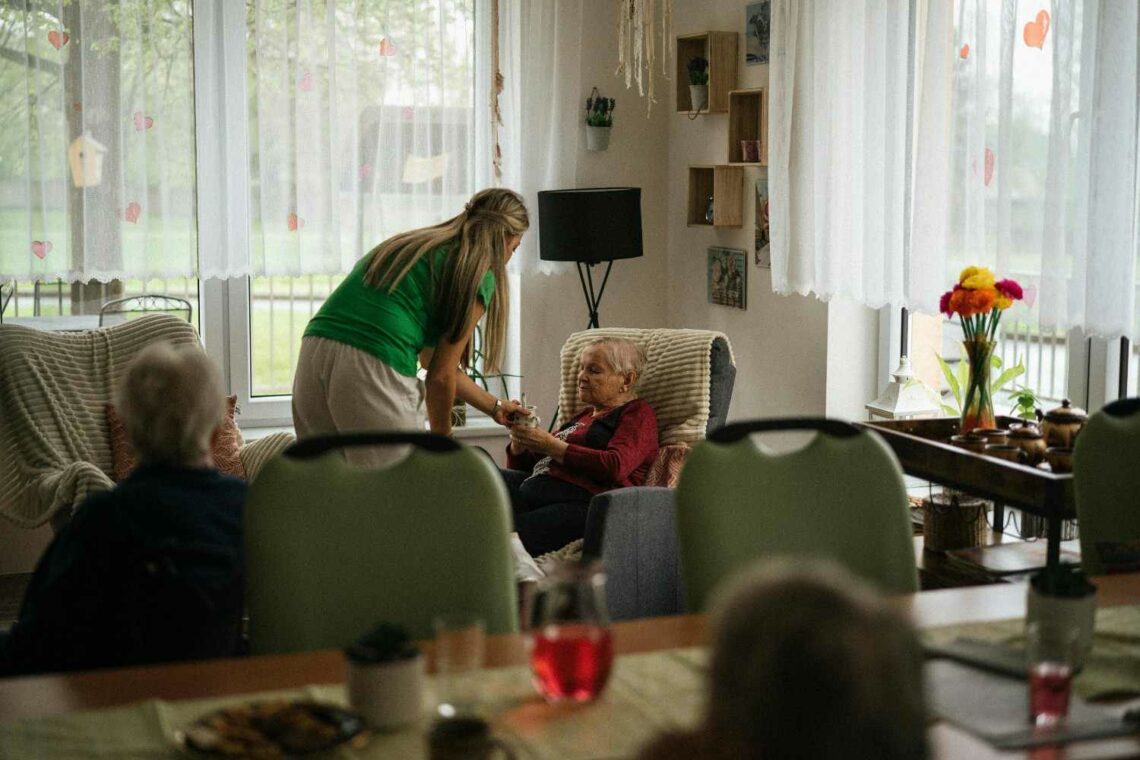
Worried about a parent living with dementia? These 10 signs suggest it may be time to consider professional dementia care at home.
Recognising when professional dementia care is needed is one of the most difficult decisions a family faces. If someone close to you is living with dementia, you may have noticed changes that concern you: moments that feel like more than ordinary forgetting, or situations at home that are becoming harder to manage safely. Knowing when those changes add up to something that needs dedicated support can make a real difference, both for the person you care about and for you.
Need Help Arranging Live-In Care?
Speak to our clinically-led team to find the right carer for your loved one. We'll guide you through costs, care options, and next steps.
Key Insights
- Repeated safety incidents at home, such as leaving the hob on or getting lost in a familiar neighbourhood, are among the clearest signals that current support is no longer enough
- Medication errors are common and serious: missed doses or accidental double-dosing can cause rapid physical deterioration in someone living with dementia
- Family caregiver exhaustion is not a personal failing; it is a clinical signal that the level of support needed has exceeded what one household can sustainably provide
- Professional dementia care at home preserves familiar surroundings and routine, which is well-evidenced as important for the wellbeing of people living with dementia
Why does timing matter when considering dementia care?
Dementia is a progressive condition. The care needs of someone in the early stages are very different from those in the later stages, and the transition from family support to professional care rarely happens in a single moment. It tends to emerge gradually, through a series of incidents and changes that, viewed together, indicate that the current level of support no longer meets the person’s needs.
According to the Alzheimer’s Society, around 982,000 people are living with dementia in the UK. Many are supported at home by family members managing extraordinary levels of daily responsibility, often without the clinical knowledge or physical capacity to do so safely over time. Exploring what dementia support services are available is a useful early step for any family in this position.
Recognising the signs early gives families more options and more time to arrange the right care. The signs below are not a clinical diagnosis. If you are concerned about a family member’s cognition or safety, a GP assessment is always the right first step. They are, however, the patterns that experienced dementia care professionals and clinical teams consistently identify as the moment when dedicated support becomes important.
What are the early signs that it’s time to consider professional dementia care?
Sign 1: Repeated safety incidents at home
Leaving the hob on, forgetting to lock the front door, or being found outside in confusion are not isolated oversights. They are safety signals. When incidents like these become a pattern rather than a rare occurrence, the home environment is no longer being managed safely without consistent, skilled oversight. There is detailed guidance on safety in dementia home care that outlines what a well-supported home environment looks like in practice.
Key incidents to watch for include:
- Leaving gas hobs, ovens, or electrical appliances on unattended
- Unlocked doors or windows, particularly at night
- Evidence of falls or near-misses around the home
- Being found outside, confused, or at an unexpected time of day
A vetted live-in carer provides the continuous presence needed to prevent these situations from escalating, something that visiting care or family support alone cannot reliably guarantee.
Sign 2: Medication errors are happening regularly
Managing medication in dementia is complex. The Alzheimer’s Society notes that people living with dementia may forget to take their medication, take it twice, or become confused about which tablet is which. For people who also have conditions such as heart disease or diabetes alongside dementia, these errors carry serious health risks.
Hometouch carers follow structured medication management plans and work within a framework of ongoing clinical supervision, providing reliable oversight that occasional family visits cannot replicate.
Sign 3: Personal hygiene and self-care have noticeably declined
Resistance to bathing, wearing the same clothes for extended periods, or difficulty with personal grooming can all reflect cognitive decline rather than personal preference. These changes are often distressing for family members to address and can create real tension, particularly when a parent refuses help altogether.
A professional carer is trained to support personal care with sensitivity and skill, approaching these tasks in ways that preserve dignity and reduce distress for everyone involved.
Sign 4: Eating and drinking have become unreliable
Dementia affects appetite, food recognition, and the routine of mealtimes. A parent who was previously a capable cook may stop preparing food regularly, forget to eat, or lose significant weight over a matter of weeks. Weight loss in dementia can accelerate physical decline, and the changes to eating and appetite that many people experience are closely connected to the neurological progression of the condition. Fluid and diet management requires close daily attention that family visits alone cannot consistently provide.
Signs to look for during visits include:
- An empty or spoiled fridge
- Uneaten meals or food left out for extended periods
- Noticeable weight loss or changes in appearance
- Difficulty recognising or preparing familiar foods
A professional carer ensures consistent, nutritious meals are prepared and that mealtimes are structured and supported throughout the day.
Sign 5: Wandering or becoming disoriented in familiar places
Wandering affects a significant proportion of people living with dementia and carries serious risks, including falls, road traffic incidents, and cold exposure. If a family member has been found outside confused, has left the house at night, or has become lost in a neighbourhood they have known for decades, the current arrangements are not providing the level of safe oversight they need.
Managing wandering requires both environmental adjustments and consistent, attentive care throughout the day and night. Practical changes to the home environment can reduce risk significantly when combined with professional care.
A dedicated live-in carer provides the continuous presence and familiarity that reduces the anxiety driving many episodes of wandering in the first place.
Sign 6: Significant mood or personality changes are affecting daily life
Anxiety, agitation, low mood, and uncharacteristic irritability are all recognised features of dementia progression. These changes can be unsettling for families and challenging to manage at home, particularly when they include verbal aggression or distress that surfaces repeatedly. Understanding why aggressive behaviour occurs in dementia helps families respond in ways that reduce rather than escalate distress.
Sundowning is a related pattern: the increased confusion and agitation many people living with dementia experience in the late afternoon and early evening. The neurological basis of sundowning is well-documented, and a trained carer understands how to adapt routines and the environment to manage it effectively.
Sign 7: The person is regularly confused about time, place, or familiar people
Disorientation that extends to not recognising a family home, believing it is a different decade, or occasionally not recognising close relatives is a feature of moderate dementia progression. Understanding how Alzheimer’s disease develops helps families recognise where their family member currently is and what level of support is appropriate.
Continuity of care matters considerably at this stage. A single dedicated carer who sees the person every day builds the kind of relationship that provides genuine reassurance and stability, rather than the disorientation that can come from a rotating roster of unfamiliar faces. The advantages of a consistent live-in carer are particularly pronounced for people at this point in their dementia journey.
Sign 8: You are visiting more frequently and finding problems each time
If you are making increasingly frequent visits to a parent and regularly discovering evidence that things have gone wrong, this is a pattern that speaks for itself. Common findings include:
- Unpaid bills or unopened post piling up
- Untouched meals or food that has been prepared incorrectly
- The house in an uncharacteristic state of disarray
- Evidence of a fall or accident that was not reported
Families caring for a parent from a distance face particular risks in this situation. The gap between what the person is managing between visits and what their needs actually require is widening, and professional support can close that gap reliably.
Sign 9: You or another family member is showing signs of carer exhaustion
Families often overlook their own wellbeing when supporting a parent with dementia. The signs of unsustainable caring are worth recognising in their own right:
- Persistent exhaustion that does not improve with rest
- Anxiety or low mood that is directly connected to the caring role
- Disrupted sleep, particularly if the person being cared for is awake at night
- Withdrawal from your own work, relationships, or health needs
- A feeling that you are never doing enough, however much you give
Arranging professional support is not a withdrawal of family involvement. Many families find that maintaining their relationship with a parent becomes easier once the daily caring responsibilities are shared with a professional. For families who are not yet at the point of needing full-time support, understanding what respite care involves is a useful step.
Sign 10: A healthcare professional has raised concerns
A GP, district nurse, community psychiatric nurse, or social worker flagging concerns about a person’s safety or self-care at home should be taken seriously. These professionals see patterns across many individuals and are not raising concerns lightly. If a clinical assessment has indicated that current support is insufficient, finding the right dementia carer should become an urgent priority rather than something to consider in the future.
It is also worth understanding at this point what NHS Continuing Healthcare funding involves, as a clinical assessment may open the door to funded care that many families are not aware of.
What does professional dementia care at home involve?
Professional dementia care at home means a trained, vetted carer living with the person or providing consistent daily support, enabling them to remain in their own home surrounded by familiar possessions, routines, and community.
Hometouch was founded by Dr Jamie Wilson, an NHS dementia specialist, and clinical oversight is embedded in how every care arrangement is structured and monitored. Understanding what a live-in carer actually does day-to-day helps families visualise what this would look like in practice.
Carers are individually matched to the person they support, not assigned from a rota, and are selected by the family after a careful matching process. The process of finding the right dementia carer is one that Hometouch’s clinical team guides families through at every step.
For families comparing options, the differences between live-in dementia care and a care home are worth understanding clearly before making any decisions. The question of how to fund live-in care is often the next consideration, and there are more options available than many families realise.
For families who have been managing alone, the introduction of a dedicated carer also means regular clinical communication and the confidence that early signs of deterioration will be identified and escalated appropriately. Hometouch is CQC-regulated and doctor-founded, with clinical governance built into every care arrangement from the start.
If you are concerned about a family member’s safety or wellbeing at home, speaking to Hometouch’s clinical team is a straightforward first step. There is no obligation. It is simply a conversation to help you understand the options available.
Frequently asked questions
What are the first signs that someone with dementia needs professional care?
The earliest signs that professional care may be needed include repeated safety incidents at home, missed medication, declining personal hygiene, and increasing disorientation. No single incident defines the threshold. It is the pattern of changes over time that indicates the current level of support is no longer meeting the person’s needs. A GP assessment should accompany any concerns about a family member’s safety or cognitive decline.
Is it possible to arrange professional dementia care at home rather than moving to a care home?
Yes. Professional live-in dementia care means a trained, vetted carer supports the person in their own home, preserving familiar surroundings, routines, and independence. For many people living with dementia, remaining at home with consistent professional support is a clinically appropriate and preferred option. The right care arrangement depends on individual needs and should be discussed with a GP and a specialist care team.
How do I know if my family member’s safety at home is at risk?
Key indicators include leaving appliances on unsupervised, leaving the property confused or at night, becoming lost in familiar areas, and being unable to manage medication or meals reliably. If you are finding evidence of these incidents during visits, or if a healthcare professional has raised safety concerns, it is worth discussing current care arrangements with a professional without delay.
What is the difference between a family carer and a professional dementia carer?
A professional dementia carer is trained in dementia communication, behaviour, medication management, and safe personal care. They bring clinical knowledge and emotional resilience that most family members, however dedicated, are not trained to provide. A professional carer also enables family members to maintain a relationship with the person rather than a purely caregiving role, which benefits everyone involved.
Can professional dementia care help with behavioural changes like aggression or wandering?
Yes. Trained dementia carers understand the neurological basis of behavioural changes such as agitation, aggression, and wandering, and are equipped to respond in ways that reduce distress rather than escalate it. Environmental adjustments, structured routines, and a consistent carer relationship all play an important part in supporting someone whose behaviour has become harder to manage at home.
Deciding that professional dementia care is needed is rarely a single moment. It is the accumulation of signs that the person you care about needs more consistent, specialist support than the current arrangements can provide. Recognising those signs early gives everyone more time, more choice, and more stability. If several of the signs in this article feel familiar, speaking to a clinical team that understands what professional dementia care at home involves is the most useful next step.
Hometouch is doctor-founded and CQC-regulated. Every care arrangement is built around the individual, clinically overseen, and supported by a team with specialist dementia expertise.
Speak to Hometouch’s clinical team today. No pressure, just answers.